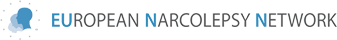Symptoms of narcolepsy
Core symptoms are excessive daytime sleepiness (EDS) and cataplexy. EDS is often the symptom that first occurs. Cataplexy can then develop after months or years.

By courtesy of the American Narcolepsy Association
Excessive daytime sleepiness
Narcolepsy is better characterized by an inability to remain awake than by an increased sleep need. EDS can occur at any time throughout the day, particularly in monotonous situations. Sleep episodes are typically irresistible, usually short and refreshing. They are often associated with dreaming. Short naps have a refreshing capacity in the majority of people with narcolepsy, in contrast to hypersomnolences other than narcolepsy. EDS is typically accompanied by a pronounced difficulty to concentrate and to sustain attention during wakefulness, leading to an impaired performance. This expression of EDS may even cause more problems in interpersonal relationships than the sleep attacks. A subject seemingly awake, but not able to perform, will receive less compassion than one who is not able to perform because being clearly asleep.
Cataplexies
Cataplexy is almost pathognomonic for narcolepsy, in that it proves the diagnosis. It is defined as a sudden loss of muscle tone triggered by strong emotions, which are mainly positive (e.g. laughter, surprise, positive anticipation etc.). Cataplexy can appear in many different forms. Sometimes it is a partial attack, limited to facial muscles (head dropping, a jaw tremor, slurred speech) or to the arms or legs (dropping of objects or buckling of the knees). It can also be a complete attack, resulting in falls.

By courtesy of Overeem / Lammers
The duration of cataplexy can last from seconds to several minutes, with a mean of two minutes. The frequency of cataplexy varies from less than one episode per year to several episodes per day. Cataplexy can be provoked by watching funny movies or by being tickled by a known person.
Hypnagogic hallucinations
Hypnagogic hallucinations can appear while falling asleep (hypnagogic) or while waking up (hypnopompic) and can be auditory, visual, haptic or sensory (feeling something creeping under the cover, feeling of being touched, smelling something is burning etc.). The term hallucination is actually not quite correct as it implicates that one is convinced that the sensation is real. However, in narcolepsy people can easily distinguish this symptom from a real perception.

Sleep paralysis
Sleep paralysis is an inability to perform voluntary movements while falling asleep or on awakening. During these episodes patients are mentally awake. Sleep paralysis can be associated with hypnagogic hallucinations. Sleep paralysis can last from a few seconds up to several minutes in rare cases.
Automatic behaviours
Automatic behaviour is characterized by continuation of an activity despite sleepiness or falling asleep. Patients are so sleepy that they cannot recall what happened during these episodes. Whether automatic behaviour is caused by ‘microsleep’ or by cognitive impairment due to sleepiness is unknown.
Nocturnal sleep
Fragmented nocturnal sleep often develops later in the course of narcolepsy and is characterized by frequent awakenings lasting minutes to hours. The total sleep time in the 24 hour period is not prolonged.
Increased body weight
Patients with narcolepsy often present with increased body-mass indices. The increase in weight often appears and remains stable after disease onset. Some people with narcolepsy, especially children, gain weight after the onset of the disease.
Associations with other sleep disorders
Non-REM parasomnias (sleepwalking, sleep terror and sleep talking) and REM parasomnias (REM sleep behaviour disorder, RBD; in which patients physically enact their dreams) have been described in 20-60% of narcoleptic patients. Many patients also suffer from sleep apnoea, periodic limb movement in sleep (repetitive, stereotyped movement of feet and toes) and some have restless legs syndrome (an urge to move the feet during wakefulness and sleep associated with unpleasant feelings of the limbs that are relieved by moving the feet).